7 Ways that Chronic Pain Changes the Brain:
-
An automated meta-analysis of 420 imaging studies – pain’s effect on the brain.
neurosynth.org uses functional connectivity and coactivation mapping from thousands of MRI images (each comprised of many cuts of images) are automated to show a final result of pain’s effect on the brain. Created and maintained by Tal Yarkoni. Supported by NIH Grant R01MH096906.

2. Chronic back pain. Touch-pain circuits shape-shift to emotional circuits.
Hashmi JA, Balike MD, Baria AT, et al. Shape shifting pain: chronicification of back pain shifts brain representation from nociceptive to emotional circuits. Brain. 2013 Sep; 136(Pt 9): 2751-2768. https://www.ncbi.nlm.nih.gov/pubmed/23983029

3. Chronic back pain. Structural changes in the brain are hard-wired, predicting who will develop it after one year.
Mansour AR, Baliki MN, Huang L, et al. Brain white matter structural properties predict transition to chronic pain. Pain. 2013 Oct; 154(10): 2160-2168. https://www.ncbi.nlm.nih.gov/pubmed/?term=10.1016%2Fj.pain.2013.06.044

4. Chronic pelvic pain. Causes microstructural changes in brain areas in how pain is felt, and how it is processed.
Woodworth D, Mayer E, Leu K, er al. Unique microstructural changes in the brain associated with urological chronic pelvic pain syndrome (UCPPS) revealed by diffusion tensor MRI, super-resolution track density imaging, and statistical parameter mapping: A MAPP Network neuroimaging study. PLoS One. 2015 Ovt 13; 10(10):e0140350. https://www.ncbi.nlm.nih.gov/pubmed/?term=Microstructural+changes+with+chronic+prostatitis%2Fchronic+pain+syndrome

5. Chronic Regional Pain Syndrome (CRPS). In “the suicide disease“, inattention in near space may occur together with distorted body perception.
Janet H. Bultitude, Ian Walker, Charles Spence; Space-based bias of covert visual attention in complex regional pain syndrome. Brain 2017 awx152. doi: 10.1093/brain/awx152 https://academic.oup.com/brain/article-lookup/doi/10.1093/brain/awx152 doi: 10.1093/brain/awx152

6. Chronic Pain. Vulnerability to develop a painful condition relates to two brain regions: the reward-motivation and the Descending Pain Modulatory System (DPMS).
Denk F, McMahon SB, and Tracey, I. Pain vulnerability: a neurobiological perspective. Nature Neuroscience 2014: 17, 192-200. http://www.nature.com/neuro/journal/v17/n2/full/nn.3628.html

7. Chronic pain and depression. Various drugs act at different sites in the cascade of neuroplasticity that cause chronic pain to develop into depression.
Shang J, Liu S, Wang Y, Cui R, and Zhang X. The Link between depression and chronic pain: neural mechanisms in the brain. Neural Plast. June 19, 2017; 9724371. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5494581/
-
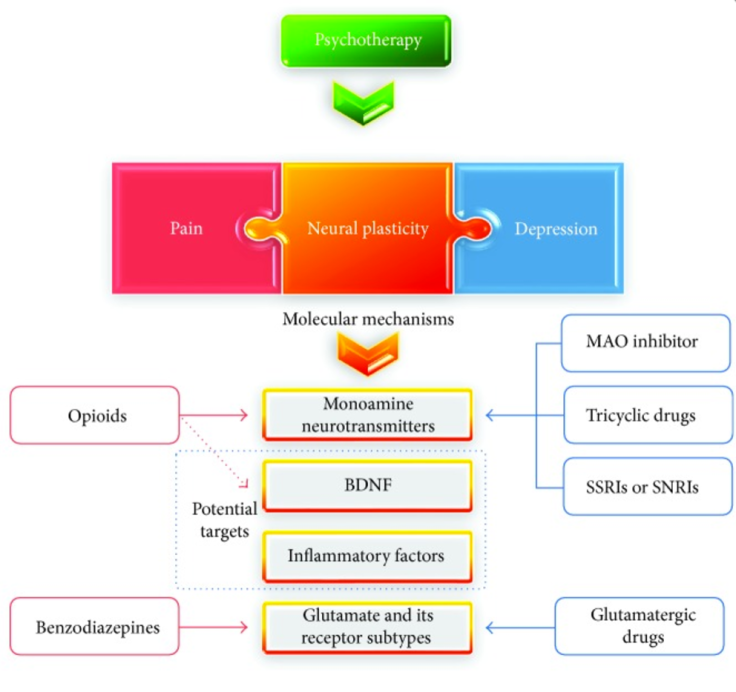
The Link between Depression and Chronic Pain: Neural Mechanisms in the Brain.
It is clear that pain changes the brain. From the last study, released on June 19, 2017, one sees the importance of neuroplasticity that modulates pain input to the brain. Pain leads to depression, which can then feed back to make the pain worse. These molecular mechanisms can be modified by opioids, benzodiazepines, MAO inhibitors, tricyclic drugs, serotonin-receptor inhibitors, and glutamatergic drugs.
# # #
THE END
# # #

Additional Articles by Dr. Margaret Aranda
Organic Orange Blueberry Scones
Organic Blueberry Buttermilk Muffins
10 Health Benefits of the Low-Glycemic Diet
Chronic Metabolic Syndrome is Killing US
7 Ways that Chronic Pain Changes the Brain
What Matters to You: Patient Advocacy
From Dr. Forrest Tennant: Hyperalgesia: No Reason to Stop or Reduce Opioids
~ ~ ~
Read Dr Margaret Aranda’s Memoirs:
Age 1: A Baby in the Sky for Father’s Day
Age 2: The Making of a Woman Intensivist
Age 6: Glistening in the Moonlight
Age 7: The Pigeon Boy, The Suction Bush and The Darkness
Age 9: Sitting on the Edge of a Cave
Age 10: Mr Bubble Strikes Again
~ ~ ~
Follow Me: Let’s Tweet and be a FB Caring Friend, too!
LIKE my Public Figure FB Page if you will, please!


Interesting. Thanks for sharing this
LikeLiked by 1 person
Thank you and the only reason I was able to write this was by having a traumatic brain injury myself. Mine was a car accident – was T-boned by a lady who lost control of her car. I’m happy to be alive. Appreciate your kind comment!
LikeLiked by 1 person
Sorry, to hear about your accident. When life altering incidents occur, things like that happen we learn to appreciate life. Be well. Have a great week,
LikeLiked by 1 person
Thank you so much for your kindness! You take care and have a fantastic week!
LikeLike